 ED: Choosing one contraceptive method that is right for a woman requires some clinical cunning and knowledge of the patient.
ED: Choosing one contraceptive method that is right for a woman requires some clinical cunning and knowledge of the patient.
How can we help patients choose a contraceptive method, given their very different priorities and needs?
Early on in a contraceptive consultation, it’s helpful to assess for contraindications to any of the possible methods, and to check for medication interactions. Specific questions need to be asked about such issues as migraine with aura (absolute contraindication to combined methods), or uterine fibroids (possible contraindication to IUD), and over the counter preparations such as St Johns wort, as these are not necessarily identified by patients.
Some factors involved in making a choice of contraceptive method include:
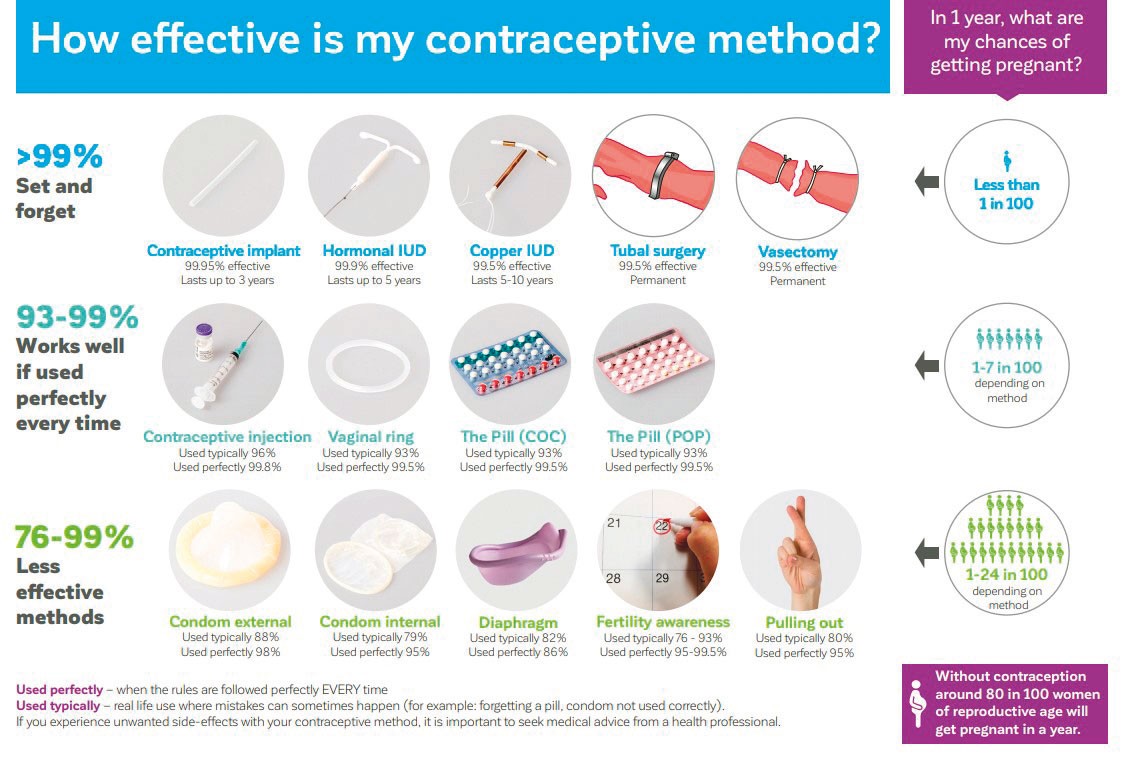
- Effectiveness
- Possible side effects – or myths about side effects
- Other benefits, such as assisting with acne, premenstrual problems or heavy menstrual bleeding
- Cost & accessibility

To help patients to make a choice, it is worth exploring these issues. For example, for Susanne a pregnancy would be a disaster, and she wants something highly effective but reversible. Implants or IUDs might become her preferred options. Marianne wants good contraception, but has awful heavy periods, so a hormonal IUD, combined pill or ring, or even a depot injection, could meet both of her needs. Part of this discussion can address any commonly held myths, of which there are plenty! Common myths include that hormonal contraception causes weight gain (there is no evidence for this – apart from depot injections!), or that IUDs are unsafe for those who are nulliparous (safety is equivalent for nulliparous and multiparous people).
Contraceptive cards, such as the recently updated Family Planning Association (FPAA) card, can be used to demonstrate the available options, ranked in order of efficacy. It is available at: https://shq.org.au/download/contraceptive-card/?wpdmdl=2085
It may be helpful to provide “potted summaries” of the methods of interest to a patient e.g. “the copper IUD is very effective, lasts for 5-10 years, and has no hormones in it. However, sometimes periods can be heavier or more painful, and the insertion can be painful.”
Using the card helps us to show patients the Long Acting Reversible Contraceptive methods, or LARCs, as the first-line options, due to their approximately twenty times greater effectiveness compared to the shorter acting options.(1) If people decide to use a shorter acting method, it’s helpful to discuss how to maximise effectiveness e.g. “What’s going to be the best way for you to remember to take your pills on time?” Strategies may include reminders in phones, or putting pills next to the bed or the toothpaste.
Once the choices have been narrowed down, additional information can be provided, such as how to use the method to obtain maximum efficacy, how to obtain the method (or the insertion process), and other important benefits and risks.
Be aware the short acting methods are most likely to be discontinued. It is helpful to suggest a return visit if any difficulties are encountered, and options for asking extra questions, such as the Sexual Health Helpline, can be offered: sexhelp@shq.org.au
Further Reading:
- Washington University. The Contraceptive Choice Project. Available from: http://www.choiceproject.wustl.edu/
References available on request.
Questions? Contact the editor.
Author competing interests: nil relevant disclosures.
Disclaimer: Please note, this website is not a substitute for independent professional advice. Nothing contained in this website is intended to be used as medical advice and it is not intended to be used to diagnose, treat, cure or prevent any disease, nor should it be used for therapeutic purposes or as a substitute for your own health professional’s advice. Opinions expressed at this website do not necessarily reflect those of Medical Forum magazine. Medical Forum makes no warranties about any of the content of this website, nor any representations or undertakings about any content of any other website referred to, or accessible, through this website.

