Inpatient cost surprise
A doc contacted us about a pensioner who had kept private health insurance going for security and to avoid waitlists but had then been surprised by a big co-payment for inpatient imaging. This was after being bulk billed for all outpatient services, which is what the two hospital providers in WA do at present. This circumstance is unusual but the Perth Rad spokesperson said they ask private inpatients if they are pensioners and bulk bill them. SKG said private inpatients pay a gap up to a ceiling of $750, and pensioners are not sought out. We repeatedly hear of private inpatients being surprised by pharmacy, physio or other co-payments after an inpatient episode.
How government helps
It sounds good – $16m in volunteer grants to support and encourage volunteering nationally. Eligible not-for-profit community organisations access between $1000 and $5000. Unspoken, is the zillions that carers and volunteers save the Australian Government in assisting disadvantaged and vulnerable people in our community. For these grants, the smaller you are, the more volunteers you have, the more disadvantaged people you help, the greater your chance of success. The deadline has now passed and the federal government says it will respond early September (just before the election).
Revalidation, here we go
Avant celebrates its 120th anniversary with the launch of a new advocacy program for its 60,000 healthcare practitioners and students nationally. It also released its polling of 150 GPs nationally about revalidation for Australian doctors. Although the doctor sample needed its own validation, key findings from the survey were: only 9% gave unconditional support and 65% expressed concerns about implementation; 23% opposed revalidation because current systems were adequate and 41% said current systems ensure doctors are fit to practise; similar respondents said revalidation should detect underperforming doctors as they were currently slipping through the cracks (25%, 19% respectively); half saw revalidation as a personal burden with administration, ineffectiveness and lack of support their main concerns.
Who needs patients?
It seems WA is fast becoming a Sim City. News that two of our universities have attracted serious dollars into simulation underscores its evolving role in the training of our future medical practitioners. UWA has opened a $3.7m Simulation Education Centre in Geraldton at the Combined Universities Centre for Rural Health (CUCRH) site. It will o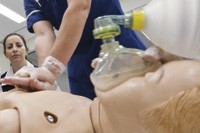 bviously be a boost for students completing clinical and community-based placements in regional areas. The ECU’s simulation centre at the Joondalup campus has just been accredited by ANZCA for the next seven years to deliver the Effective Management of Anaesthetic Crisis (EMAC) course. And when it comes to Teleheath (see our feature on P18), is there nothing that can’t be done by video. In ACRRM’s latest newsletter there were training modules form treating younger women with early breast cancer, pain management and Hep B among others.
bviously be a boost for students completing clinical and community-based placements in regional areas. The ECU’s simulation centre at the Joondalup campus has just been accredited by ANZCA for the next seven years to deliver the Effective Management of Anaesthetic Crisis (EMAC) course. And when it comes to Teleheath (see our feature on P18), is there nothing that can’t be done by video. In ACRRM’s latest newsletter there were training modules form treating younger women with early breast cancer, pain management and Hep B among others.
Penalised if you do, damned if you don’t
Which brings us to the thorny issue arising from the recent federal budget of capping CPD tax deductions (effective July1, 2014). On one hand, the government insists that doctors keep their skills sharp and up-to-date, on the other hand the tax break stops once you hit $2000. The RACGP’s president Dr Liz Marles says this will hit GPs and junior doctors the hardest. She said face-to-face activities, which had “significant advantages” in learning outcomes, were more expensive.
Mandurah still in SJOG sights
Now Ramsay has taken the helm of the Peel Health Campus from Health Solutions WA, news comes that St John of God Health Care is still forging on with its plan for its $45m private hospital nearby. Architects Silver Thomas Hanley, project managers Project Directors Australia (PDA) and cost managers Ralph Beattie Bosworth (RBB) have been appointed to work on the 75-bed hospital, which is expected to open in 2016. SJOGHC sees Mandurah’s growing and ageing population will demand more specialist services. The SJOGHC board will be presented with a financial feasibility study late this year and the decision will be taken then if the hospital will get the three green lights.
First, build your house
There’s an old show biz saying, ‘put it on stage and the crowds will come’. It’s an unreliable truism in theatre … but will it prove the deal maker in Port Hedland where seven new houses have been built specifically for GPs? The $4.5m project received money from Royalties for Regions, the Town of Port Hedland and BHP Billiton. The Minister Mr Brendon Grylls thinks the houses are essential to attract more doctors to the region. Will he be bowled over in the rush?

