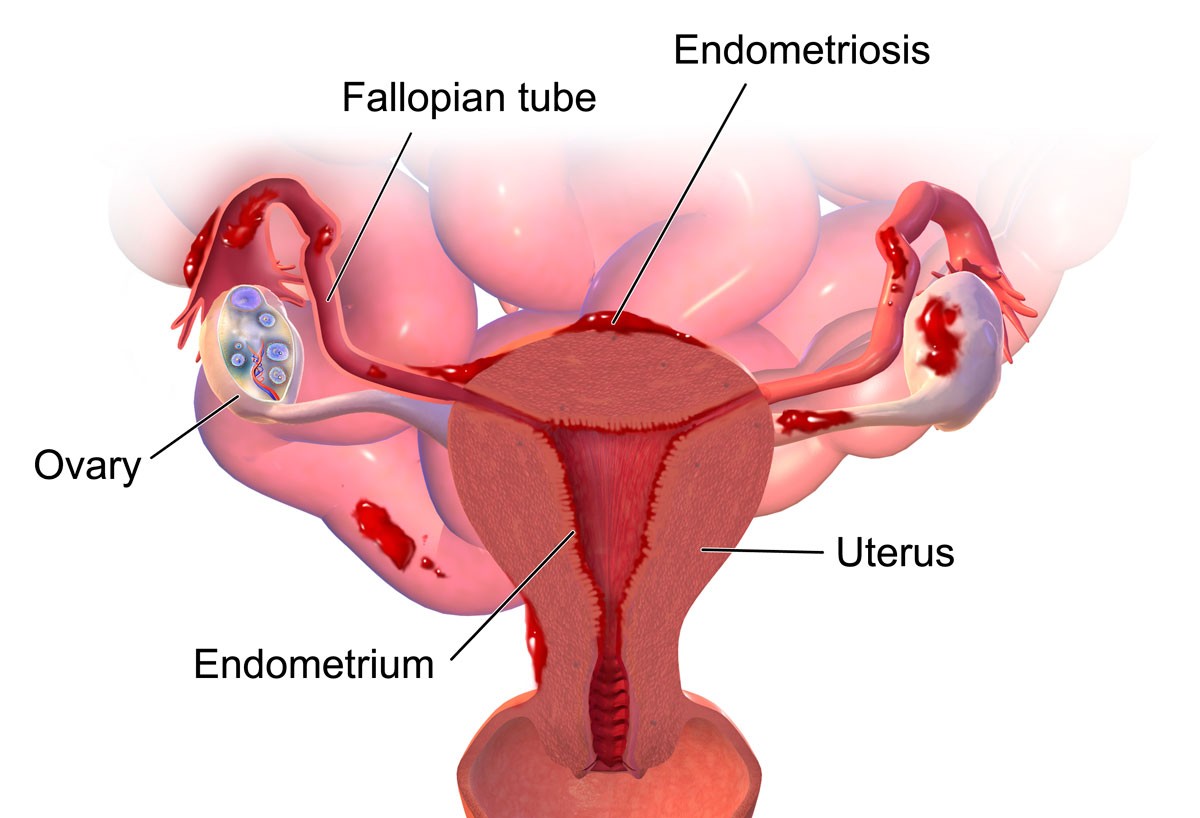
 ED: Endometriosis is a common, but under-recognised condition causing significant missed days off work and school, decreased participation in social activities and depression.
ED: Endometriosis is a common, but under-recognised condition causing significant missed days off work and school, decreased participation in social activities and depression.
Endometriosis, a chronic condition estimated to affect 700,000 Australian women and girls, occurs when cells similar endometrial cells grow on pelvic tissues and organs (and rarely outside the pelvis). These cells respond to oestrogen and progesterone in a manner similar to the endometrium resulting in bleeding, inflammation and pelvic scarring manifesting as severe dysmenorrhoea, chronic pelvic pain and subfertility
Step one in management is considering the diagnosis. Women with endometriosis frequently report years of dismissal of symptoms by doctors. Many are told period pain is normal and to learn to deal with it, that they should have a baby and their symptoms will get better, or worse – that the symptoms are a manifestation of anxiety or depression.
The Australian government announced a National Endometriosis Action Plan in July 2018 to increase awareness, streamline services, promote earlier intervention and decrease the social disruption experienced by so many women.
Suspect endometriosis in any woman reporting severe period pain, especially if leading to regular absence from school or work. Chronic pelvic pain, deep dyspareunia and infertility are also common symptoms

Routine pelvic ultrasound can diagnose endometriomas. More advanced techniques can assess for other features including site-specific tenderness and ovarian mobility, assessment of the pouch of Douglas and the presence and depth of deep infiltrating lesions. The presence of these features may prompt early referral to a specialty endometriosis service. Early involvement of such a service may avoid repeat surgeries. A normal ultrasound does not exclude endometriosis.
Laparoscopy is the mainstay of diagnosis. Where possible, a biopsy should be taken for histological confirmation. Management at the time of laparoscopy depends on the extent of the disease and the skill of the surgeon. If a woman has severe endometriosis (bilateral endometriomas, deep infiltrating disease involving bladder or bowel and / or obliteration of the pouch of Douglas), she should ideally be referred to a tertiary centre for multidisciplinary involvement. This team may include a gynaecologist with skills in advanced laparoscopy, a colorectal surgeon, fertility specialist, pain specialist and a gynaecology specialist nurse. Inappropriate management of endometriomas can damage the ovary significantly impacting future fertility.
Hormonal manipulation can manage endometriosis pain. The pill can be taken either cyclically or continuously. An intrauterine levonorgestrel device can be very effective for chronic pain. Intra-muscular long acting progesterone is effective but often disliked due to the side effect of irregular bleeding.
Gosarelin implants are PBS listed for a once off, six month course for histologically proven endometriosis. The disadvantages are menopausal-type side effects.
The psycho-social impacts of this condition are important. Information and support groups are available.
Key Messages
- Endometriosis is common, affecting 10% of Australian women and girls
- Refer women with severe endometriosis to a specialist endometriosis service
- The psychosocial impact of endometriosis is significant
References available on request.
Questions? Contact the editor.
Author competing interests: nil relevant disclosures.
Disclaimer: Please note, this website is not a substitute for independent professional advice. Nothing contained in this website is intended to be used as medical advice and it is not intended to be used to diagnose, treat, cure or prevent any disease, nor should it be used for therapeutic purposes or as a substitute for your own health professional’s advice. Opinions expressed at this website do not necessarily reflect those of Medical Forum magazine. Medical Forum makes no warranties about any of the content of this website, nor any representations or undertakings about any content of any other website referred to, or accessible, through this website.
Image credit:

