 Most people would be familiar with the story of Tiger Woods having years of intense therapy, ‘core’ exercises, back taping, medications, spine injections and four back surgeries for his back pain. Despite some symptom reduction, his back pain remains ongoing and limiting.
Most people would be familiar with the story of Tiger Woods having years of intense therapy, ‘core’ exercises, back taping, medications, spine injections and four back surgeries for his back pain. Despite some symptom reduction, his back pain remains ongoing and limiting.

According to the International Olympic Committee, athletes are commonly managed by rest, limited training and competition, early referral for diagnostic imaging, and treatments targeting symptom reduction, correction of faulty structures and ‘fixing’ damaged tissue. This approach is not aligned to current best practice guidelines for the management of musculoskeletal (MSK) pain.
The assumption that MSK pain associated with sport is a sign of tissue damage, makes sense in traumatic injury with clear identifiable symptoms, where temporary protection and rest of the injured area is needed for healing to occur, before rehabilitation and return to sport.
However, MSK pain, in the absence of trauma, is commonly managed with early scanning, over-treatment and advice to limit activities presumed to be dangerous. This can lead to reduced confidence and fear of injury, vigilance and deconditioning, which increases the risk of pain and chronicity.
Modern understanding of pain goes beyond structural considerations. The degree of tissue damage on imaging is a poor measure of a person’s pain, distress and disability. Imaging findings such as disc degeneration, disc bulges, hip labral tears, rotator cuff tears, meniscal tears, and tendinopathy are prevalent in pain-free athletic populations, and are a poor predictor of a person’s risk of future pain and activity limitation.
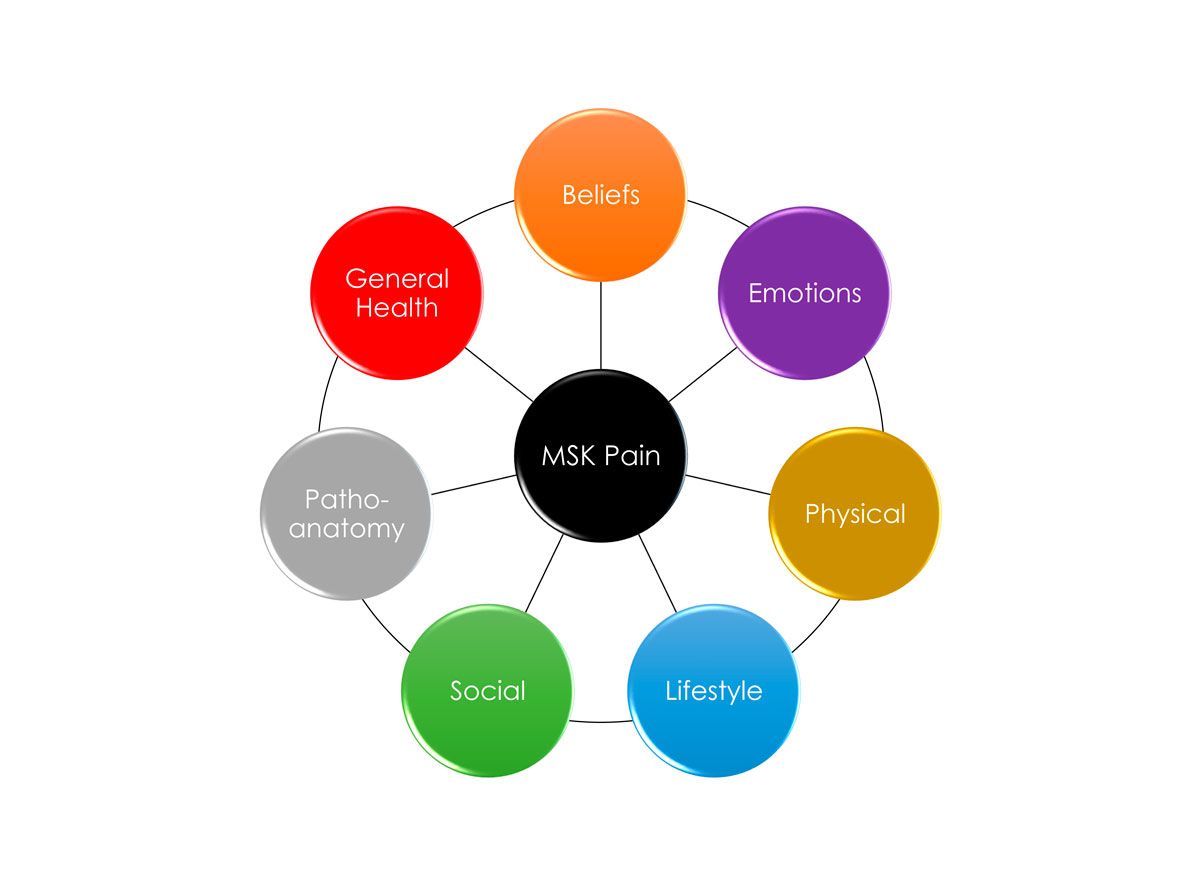 The development of non-trauma MSK pain in athletic populations is better predicted by factors such as sudden increases in training volume, poor sleep, fatigue, and depressed mood than structural factors. The strongest predictors of MSK pain chronicity and disability are avoidance of movement and activity, pain-related distress, and low self-efficacy.
The development of non-trauma MSK pain in athletic populations is better predicted by factors such as sudden increases in training volume, poor sleep, fatigue, and depressed mood than structural factors. The strongest predictors of MSK pain chronicity and disability are avoidance of movement and activity, pain-related distress, and low self-efficacy.
A new approach is needed
Over-treatment of sport-related pain complaints can be reduced. In the absence of trauma, do not assume that pain indicates tissue injury. Do not misinterpret age-related changes on imaging for pathology. Consider, screen for, and manage the athlete’s overall physical and mental health as well as training-related factors to improve function, pain and sports participation.
Physical activity is safe and protective so keep athletes training as tolerated. Use symptom palliation (passive therapies, medication, injections) only as an adjunct to active management (education, physical activation, lifestyle changes).
For non-traumatic MSK pain, only use evidence-based surgical interventions that are supported and when evidence-based non-surgical interventions have been trialled. Use shared decision making to devise an individualised treatment plan. Empower athletes to develop skills to self-manage possible flare ups. Implementing best care practice principles is likely to reduce over-treatment in sports.
Acknowledgement: The author acknowledges the input of Prof Peter O’Sullivan.
Key messages
- Musculoskeltal pain in the absence of trauma does not equal tissue damage
- Address any underlying physical and mental health contributors
- Encourage self-management
References available on request.
Questions? Contact the editor.
Author competing interests: nil relevant disclosures.
Disclaimer: Please note, this website is not a substitute for independent professional advice. Nothing contained in this website is intended to be used as medical advice and it is not intended to be used to diagnose, treat, cure or prevent any disease, nor should it be used for therapeutic purposes or as a substitute for your own health professional’s advice. Opinions expressed at this website do not necessarily reflect those of Medical Forum magazine. Medical Forum makes no warranties about any of the content of this website, nor any representations or undertakings about any content of any other website referred to, or accessible, through this website.

